Liver Transplant in Turkey
Liver Transplant in Turkey
A Complete Medical Guide for International Patients: Who Needs It, When It’s Required, and Why Turkey Leads Globally
Over the last two decades, Turkey has become one of the world’s most advanced destinations for liver transplantation. This transformation did not happen overnight. It reflects years of investment in medical infrastructure, surgeon training, donor programs, and international patient services.
Today, Turkey offers a comprehensive liver transplant ecosystem that combines:
-
Highly specialized transplant surgeons
-
Advanced surgical and ICU technologies
-
Strong living-donor programs
-
Rapid evaluation pathways
-
Structured post-transplant follow-up
For patients from the Middle East, Europe, and North Africa, Turkey represents not only access to life-saving surgery — but also continuity of care, affordability, and medical excellence.
This multi-part guide is designed to help patients and families clearly understand:
-
What liver transplantation is
-
Who needs it
-
When it becomes medically unavoidable
-
Why Turkey has emerged as a global leader
-
How professional medical guidance improves outcomes
What Is a Liver Transplant?
A liver transplant is a highly complex surgical procedure in which a diseased liver is replaced with a healthy liver obtained from either:
-
A deceased donor (whole liver)
-
A living donor (partial liver)
The liver has a unique regenerative capacity, allowing both donor and recipient to regain functional liver volume after surgery. This biological property makes living-donor transplantation possible and safe when performed under strict medical protocols.
A transplant becomes necessary when the liver can no longer perform essential physiological functions such as:
-
Detoxification of blood
-
Regulation of metabolism
-
Production of clotting factors and proteins
-
Bile secretion for digestion
Once liver failure reaches an advanced stage and medical therapy is no longer effective, transplantation becomes the only curative option.
Who Needs a Liver Transplant?
Liver transplantation is recommended for patients suffering from irreversible liver damage or selected liver cancers.
The most common indications include:
1. End-Stage Liver Disease
This includes advanced cirrhosis caused by:
-
Chronic viral hepatitis (B or C)
-
Non-alcoholic fatty liver disease (NAFLD/NASH)
-
Autoimmune hepatitis
-
Alcohol-related liver disease
-
Cryptogenic cirrhosis
At this stage, patients often experience complications such as ascites, jaundice, gastrointestinal bleeding, encephalopathy, and muscle wasting.
2. Primary Liver Cancer
Especially hepatocellular carcinoma (HCC) within accepted transplant criteria (such as Milan criteria).
Unlike tumor resection alone, transplantation removes both:
-
The cancer
-
The diseased liver environment that promotes recurrence
This makes transplant a definitive oncologic and functional cure in carefully selected patients.
3. Genetic and Metabolic Liver Disorders
Including:
-
Wilson’s disease
-
Alpha-1 antitrypsin deficiency
-
Certain pediatric metabolic syndromes
-
Congenital biliary abnormalities
Eligibility for transplantation is determined through structured clinical assessment and waiting-list prioritization following guidelines from organizations such as the American Association for the Study of Liver Diseases.
In cancer cases, doctors often apply “bridging therapies” (local tumor control treatments) to keep patients eligible while waiting for a donor organ.
When Does Liver Transplant Become Medically Necessary?
Timing is one of the most critical factors in transplantation.
Transplant should ideally occur before irreversible multi-organ damage develops, but after liver function has declined enough to justify surgery.
Physicians use scoring systems such as MELD (Model for End-Stage Liver Disease) to quantify severity and guide prioritization.
Delaying transplantation too long may lead to:
-
Kidney failure
-
Severe malnutrition
-
Recurrent infections
-
Cardiac complications
These factors significantly reduce post-transplant survival.
Early referral to a transplant program — even before absolute failure — improves long-term outcomes.
Why Turkey Has Become a Global Leader in Liver Transplantation
Turkey’s rise as a transplant powerhouse is based on several strategic advantages:
Advanced Hospital Infrastructure
Modern operating rooms, hybrid ICUs, advanced imaging, and laboratory systems support complex transplant cases with precision.
Strong Living-Donor Programs
Turkey is internationally recognized for expertise in living-donor liver transplantation, significantly reducing waiting times compared with many Western countries.
This is especially important for international patients who cannot remain on long waiting lists abroad.
Highly Experienced Surgical Teams
Turkish transplant surgeons perform thousands of liver transplants annually, including highly complex cases involving vascular reconstruction and re-transplantation.
Rapid Evaluation Pathways for International Patients
Unlike many countries, Turkey offers streamlined assessment:
-
Medical review within days
-
Fast laboratory and imaging schedules
-
Multidisciplinary committee decisions
-
Quick surgical planning
Continuous Outcome Improvement
Studies from 2023–2025 demonstrate rising survival rates and decreasing complication profiles across major Turkish transplant centers.
Together, these factors make Turkey one of the few countries able to combine:
High volume + high quality + accessibility.
The Importance of Professional Medical Guidance
While Turkey offers excellent surgical capability, outcomes depend heavily on:
-
Proper patient selection
-
Center choice
-
Pre-transplant optimization
-
Post-transplant monitoring
This is where coordinated medical supervision becomes critical.
The Role of Dr. Al-Akkad in Liver Transplant Care
A major advantage for many international patients is having a single medical reference throughout their journey.
Dr. Al-Akkad provides comprehensive medical oversight for liver transplant patients from first contact through long-term recovery.
His role includes:
-
Detailed review of medical records
-
Determination of transplant eligibility
-
Selection of appropriate Turkish transplant centers
-
Coordination of pre-transplant evaluations
-
Continuous presence during hospitalization
-
Supervision of immunosuppressive management
-
Long-term remote follow-up after patients return home
Rather than fragmented care across multiple providers, patients benefit from one physician who understands their entire medical history and guides every stage of the process.
This integrated approach significantly reduces complications, improves compliance, and offers families clarity during an otherwise overwhelming journey.
 Liver Transplant in Turkey
Liver Transplant in Turkey
Donor Types, Surgical Journey, and What Patients Experience from Arrival to Early Recovery
In Part 1, we explored who needs liver transplantation, when it becomes medically necessary, and why Turkey has become a global leader in this life-saving field.
In Part 2, we focus on the practical journey:
-
Living vs deceased donor transplantation
-
How grafts are selected
-
Donor safety principles
-
Step-by-step surgical pathway
-
What happens after arrival in Turkey
-
ICU care and early recovery
This section is designed to answer the most common questions patients and families ask before making their decision.
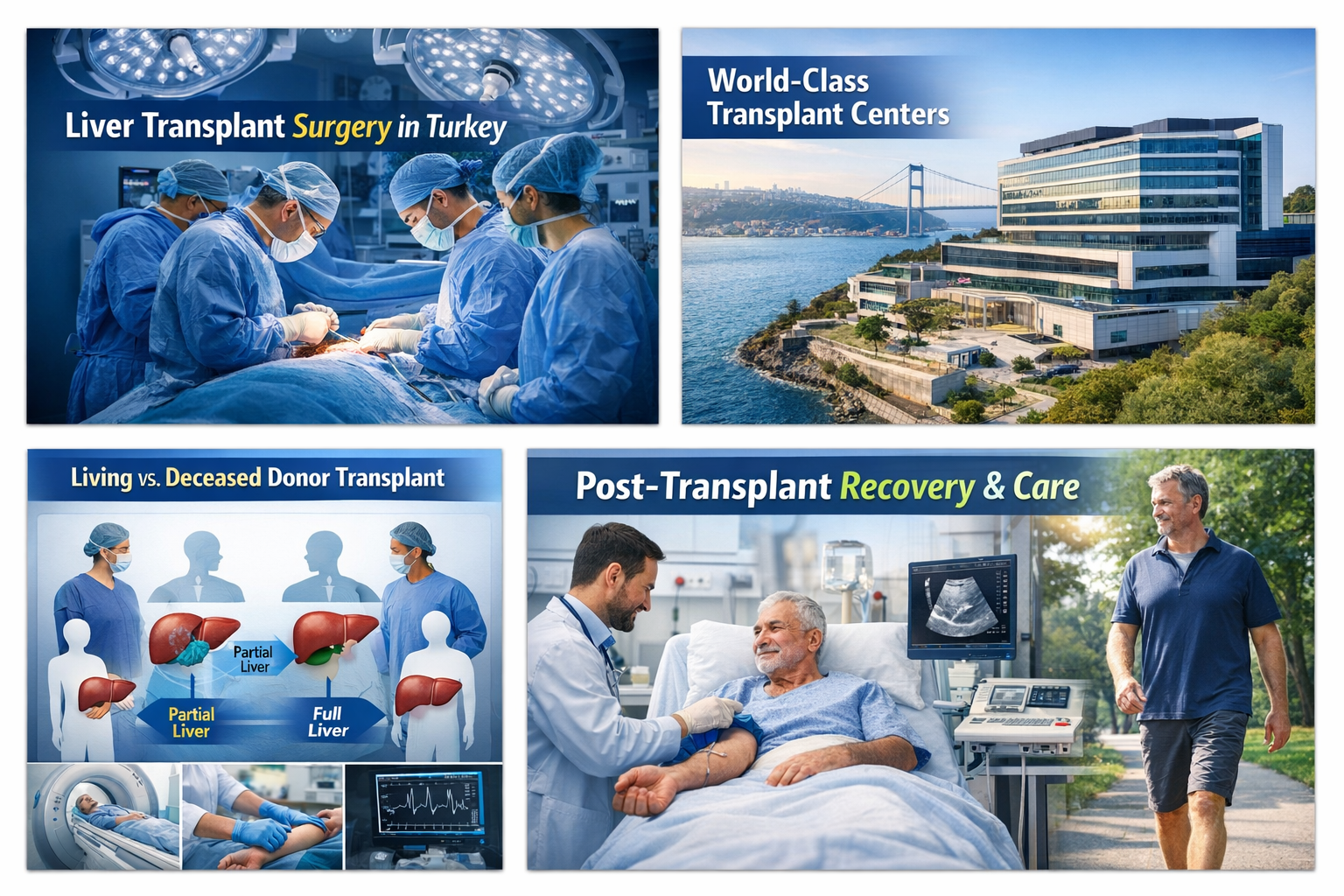
Living Donor vs Deceased Donor Liver Transplantation
There are two main pathways for liver transplantation:
Living Donor Liver Transplant (LDLT)
In this approach, a healthy relative or compatible donor gives a portion of their liver. Both donor and recipient regenerate liver volume over time.
Key advantages:
-
Shorter waiting time
-
Surgery can be scheduled electively
-
Better planning and optimization of patient condition
-
Excellent outcomes in experienced centers
Turkey is internationally recognized for its strong LDLT programs, making it especially attractive for international patients who cannot remain on prolonged waiting lists.
Deceased Donor Liver Transplant (DDLT)
Here, the entire liver is obtained from a donor who has been declared brain-dead.
Key characteristics:
-
Organ availability depends on national allocation systems
-
Timing is unpredictable
-
Suitable for patients without living donor options
In advanced Turkish centers, outcomes for deceased-donor transplants closely match those of living-donor procedures when performed by experienced surgical teams.
Which Liver Lobe Is Used in Living Donation?
When a living donor is involved, surgeons must carefully balance:
-
Maximum donor safety
-
Adequate graft size for the recipient
Modern practice increasingly favors left-lobe donation whenever anatomical measurements allow.
A large systematic review published in 2022 demonstrated that:
-
Left-lobe donors experience fewer complications
-
Recipient outcomes remain excellent provided graft volume is sufficient
For this reason, many Turkish transplant programs prioritize left-lobe grafts when feasible, reflecting their strong emphasis on donor protection.
Before surgery, advanced imaging and 3D volumetric analysis are used to calculate:
-
Donor remnant liver volume
-
Recipient graft requirements
-
Vascular anatomy
This planning phase is critical to success.
Comprehensive Pre-Transplant Evaluation
Before any surgery is approved, both recipient and donor undergo extensive assessments designed to reduce risk and improve outcomes.
These typically include:
For the Recipient
-
MELD score calculation to assess liver failure severity
-
Full blood panel and infection screening
-
Cardiac evaluation (ECG, echocardiography, stress testing if needed)
-
Pulmonary function testing
-
CT or MRI of liver and vessels
-
Nutritional assessment
-
Psychological evaluation
Patients with liver cancer may receive “bridging therapies” to maintain transplant eligibility while waiting for surgery, in line with guidance from bodies such as the American Association for the Study of Liver Diseases.
For the Living Donor
Donor safety is paramount and includes:
-
Complete laboratory screening
-
Detailed liver imaging
-
Cardiac and pulmonary testing
-
Psychological clearance
-
Independent donor advocacy review
Only donors who meet strict international safety criteria are accepted.
What Happens After Arriving in Turkey?
Once international patients arrive, most Turkish transplant centers follow a structured fast-track pathway:
Step 1: Comprehensive Medical Consultation
All previous reports are reviewed, physical examination is performed, and the treatment roadmap is explained.
Step 2: Rapid Diagnostic Testing
Blood work, imaging, and cardiac/pulmonary evaluations are typically completed within days.
Step 3: Multidisciplinary Transplant Committee
Surgeons, hepatologists, anesthesiologists, radiologists, and coordinators jointly confirm eligibility and finalize surgical planning.
Step 4: Surgery Scheduling
For living donors, surgery is scheduled once both donor and recipient are cleared.
For deceased donors, patients remain on standby until an organ becomes available.
The Surgical Procedure: Step by Step
Although each case is individualized, the general sequence includes:
-
Donor hepatectomy (for living donors)
-
Recipient liver removal
-
Implantation of the new liver graft
-
Vascular reconstruction (hepatic artery, portal vein, hepatic veins)
-
Biliary reconstruction
-
Hemostasis and closure
Operations typically last several hours and are performed by specialized transplant teams.
Immediately afterward, patients are transferred to the intensive care unit (ICU).
Intensive Care and Early Recovery
The first 48–72 hours are critical.
During ICU stay, teams closely monitor:
-
Liver function tests
-
Blood clotting parameters
-
Hemodynamics
-
Kidney function
-
Signs of bleeding or infection
Most patients are extubated within 24–48 hours and gradually transferred to regular wards as stability improves.
Early mobilization, breathing exercises, and nutritional support begin as soon as possible.
Hospitalization usually lasts between 10–21 days, depending on individual recovery.
Why Continuous Medical Supervision Matters
Successful transplantation does not depend on surgery alone.
Equally important are:
-
Pre-transplant optimization
-
Early complication detection
-
Medication management
-
Long-term follow-up
This is where coordinated medical oversight becomes essential.
The Role of Dr. Al-Akkad Throughout the Surgical Journey
A major advantage for international patients is having a single physician overseeing their entire transplant pathway.
Dr. Al-Akkad accompanies liver transplant patients from the first consultation through surgery and into recovery.
His involvement includes:
-
Reviewing medical records and determining candidacy
-
Selecting appropriate Turkish transplant centers
-
Coordinating donor and recipient evaluations
-
Remaining closely involved during hospitalization
-
Supervising early post-operative progress
-
Guiding immunosuppressive initiation
-
Ensuring smooth transition to outpatient care
-
Providing structured remote follow-up after patients return home
This integrated model offers patients continuity, clarity, and medical consistency — replacing fragmented care with a unified treatment strategy.
For many families, this single-point medical leadership provides confidence during one of the most complex journeys in modern medicine.
Liver Transplant in Turkey
Immunosuppression, Rejection Monitoring, Long-Term Outcomes, and Life After Transplant
In Parts 1 and 2, we covered who needs liver transplantation, why Turkey has become a global leader, donor options, surgical steps, and early recovery.
Part 3 focuses on what truly defines success: post-transplant care.
A liver transplant does not end in the operating room. It begins a lifelong medical partnership centered on immunosuppression, structured monitoring, lifestyle adaptation, and continuous clinical supervision.
This final section explains:
-
Immunosuppressive medication protocols
-
How rejection is detected and prevented
-
Common post-transplant complications
-
Long-term survival expectations
-
Daily life after liver transplantation
-
Updated 2025 concepts in post-transplant care
-
The importance of continuous medical oversight
Immunosuppressive Therapy: Protecting the New Liver
After transplantation, the immune system naturally recognizes the new liver as foreign. Without treatment, this would lead to rejection.
To prevent this, patients must take lifelong immunosuppressive medications.
Typical regimens include combinations of:
-
Calcineurin inhibitors (such as tacrolimus)
-
Antimetabolites (such as mycophenolate)
-
Corticosteroids (usually tapered over time)
The goal is precise balance:
-
Too little immunosuppression → rejection
-
Too much immunosuppression → infections, kidney injury, metabolic problems
Therefore, dosing is continuously adjusted based on:
-
Blood drug levels
-
Liver function tests
-
Kidney performance
-
Clinical symptoms
Early months require frequent laboratory monitoring, which gradually becomes less intensive as stability improves.
Modern protocols aim to minimize steroid exposure and reduce long-term toxicity while preserving graft function.
How Rejection Is Detected and Managed
Rejection does not always produce obvious symptoms. This is why routine monitoring is essential.
Signs may include:
-
Rising liver enzymes
-
Fatigue or fever
-
Abdominal discomfort
-
Changes in bile flow
Diagnosis is confirmed through:
-
Blood tests
-
Imaging
-
Sometimes liver biopsy
When detected early, most rejection episodes respond well to medication adjustments or short courses of intensified immunosuppression.
Current clinical recommendations — including those supported by the American Association for the Study of Liver Diseases — emphasize proactive surveillance rather than reactive treatment.
Early detection dramatically improves outcomes.
Biliary and Vascular Complications
Although modern techniques have reduced complication rates, some patients may experience:
Biliary Issues
-
Bile duct narrowing (strictures)
-
Leakage at surgical connections
These are often managed using endoscopic procedures rather than surgery.
Vascular Problems
-
Hepatic artery thrombosis
-
Portal vein narrowing
Prompt imaging and intervention usually prevent graft loss when identified early.
The key factor across all complications is speed of diagnosis, which depends on structured follow-up.
Long-Term Survival After Liver Transplant
Global data show excellent survival in properly selected patients:
-
High 1-year survival
-
Strong 3- and 5-year outcomes
-
Increasing numbers of patients living decades with functional grafts
In Turkey, outcomes in experienced centers closely match leading international programs.
Long-term success depends on:
-
Patient condition before transplant
-
Surgical expertise
-
Adherence to medication
-
Continuous monitoring
-
Lifestyle compliance
Transplantation today is no longer considered a temporary solution — it is a chronic care pathway with increasingly predictable outcomes.
Life After Liver Transplant: What Patients Can Expect
Most patients gradually return to active, productive lives.
However, success requires commitment.
Daily Medication
Immunosuppressants must be taken at fixed times every day without interruption.
Nutrition
Patients are advised to:
-
Maintain balanced protein intake
-
Limit salt
-
Avoid raw or unsafe foods
-
Stay hydrated
Alcohol is strictly prohibited.
Physical Activity
Light movement begins early. Over time, patients progress to normal activity and moderate exercise.
Infection Prevention
Because immunity is suppressed:
-
Good hygiene is essential
-
Crowded exposure should be limited early on
-
Vaccination schedules are reviewed
Mental Health
Emotional adjustment is important. Many patients benefit from psychological support during recovery.
With proper care, most recipients resume work, travel, and family life.
Updated 2025 Principles in Post-Transplant Care
Recent international trends emphasize:
-
Personalized immunosuppression
-
Reduced steroid exposure
-
Early mobilization protocols
-
Telemedicine follow-up
-
Digital lab monitoring
-
Risk-based surveillance models
These strategies improve quality of life while preserving graft longevity.
Turkish transplant centers increasingly integrate these concepts, offering modern, patient-centered recovery programs.
Why Continuous Medical Supervision Makes the Difference
Transplant medicine is not episodic. It is continuous.
Patients who lack coordinated follow-up face higher risks of:
-
Late rejection
-
Medication errors
-
Silent complications
-
Preventable hospitalizations
This is why having a single overseeing physician significantly improves outcomes.
The Role of Dr. Al-Akkad in Long-Term Follow-Up
Dr. Al-Akkad provides structured medical continuity for liver transplant patients far beyond surgery.
His role includes:
-
Ongoing review of laboratory trends
-
Adjustment of immunosuppressive therapy
-
Early detection of complications
-
Coordination with transplant surgeons when needed
-
Lifestyle guidance
-
Remote follow-up after patients return to their home countries
This unified care model gives patients one consistent medical reference who understands their entire clinical history.
Instead of fragmented care, patients receive continuous supervision from evaluation through lifelong recovery — a key factor in preserving graft function and quality of life.
Final Thoughts
Liver transplantation in Turkey combines advanced surgery with comprehensive post-operative care.
But true success comes from:
-
Correct patient selection
-
Experienced surgical teams
-
Modern medical protocols
-
Lifelong follow-up
-
Dedicated medical leadership
For international patients, this integrated approach transforms transplantation from a single operation into a sustainable new life chapter.
Begin Your Medical Evaluation
If you are considering liver transplantation in Turkey and would like personalized medical guidance or treatment planning, you may contact Dr. Al-Akkad directly for an initial consultation and professional evaluation based on your specific condition.

